

Tendon pain is one of the most common reasons people seek care—whether it’s shoulder pain when reaching overhead, elbow pain with gripping, hip discomfort when walking, or Achilles pain during activity.
And yet, despite how common it is, tendon pain is often misunderstood.
Many patients are told some version of:
- “It’s just inflammation.”
- “It’s wear and tear.”
- “You should rest it.”
While these explanations aren’t entirely wrong, they’re often incomplete—and that’s where frustration begins. Pain lingers, activity becomes limited, and recovery feels uncertain.
Let’s take a closer look at what’s really happening.
Tendons Are Not Static—They Adapt
Tendons are living, dynamic tissues. They respond to how we load them—whether that’s exercise, daily activity, or even prolonged inactivity.
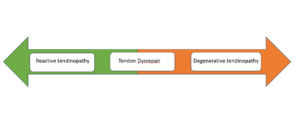
Instead of thinking of tendon pain as a single diagnosis, it’s more accurate to think of it as a continuum:
- Early stage (reactive): The tendon becomes sensitive and irritated, often due to a sudden increase in activity or load
- Intermediate stage (disrepair): The tendon begins to show changes in its structure and organization
- Later stage (degenerative): The tendon may develop more chronic changes and reduced capacity to handle stress
The key point?
Where you are on this continuum matters—and it should guide how you are treated.

Why a One-Size-Fits-All Approach Doesn’t Work
If you’ve tried rest, ice, injections, or even physical therapy and still have pain, you’re not alone.
One of the most common reasons for this is that treatment wasn’t matched to the stage of your tendon or your specific functional needs.
For example:
- A tendon that is highly sensitive may need a very different loading strategy than one that has been chronically underperforming
- Complete rest might temporarily reduce pain, but it often does not improve the tendon’s ability to handle activity
- General exercise programs may not target the underlying issue
This is why a more individualized approach is so important.
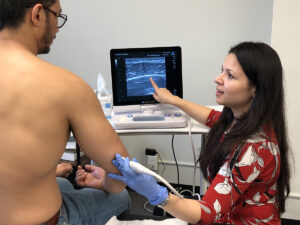
Seeing Beyond the Surface: The Role of Ultrasound
One of the most valuable tools I use in my practice is diagnostic musculoskeletal ultrasound.
Unlike static imaging, ultrasound allows us to:
- Visualize the tendon in real time
- Assess its structure and quality
- Correlate what we see with your symptoms and movement
This helps answer critical questions:
- Is the tendon acutely irritated or more chronically changed?
- Is there a mismatch between your symptoms and the tissue’s appearance?
- How does the tendon respond during movement?
This level of detail allows for a much more precise and personalized treatment plan.
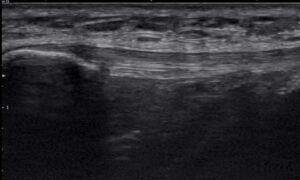
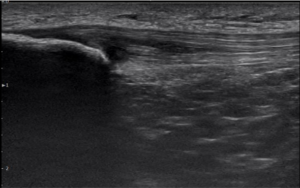
What a Better Approach Looks Like
When we truly understand your tendon, treatment becomes more focused and effective.
A comprehensive plan may include:
- Targeted loading strategies to improve tendon capacity
- Movement assessment and correction to reduce unnecessary strain
- Progressive return to activity based on how your body responds
- Ongoing reassessment, including imaging when needed
The goal is not just to reduce pain—but to restore confidence in movement and prevent recurrence.

You Don’t Have to “Just Live With It”
Tendon pain can be frustrating, especially when it limits the things you enjoy or need to do every day.
But with the right evaluation and a more precise approach, improvement is not only possible—it’s expected.
If you’ve been dealing with persistent tendon pain or feel like you haven’t gotten clear answers, it may be time to look at it differently.

Ready to Take the Next Step?
If you’d like a more in-depth evaluation and a personalized plan, I’d be happy to help.
You can learn more or schedule an appointment HERE
Dr. Mohini Rawat specializes in musculoskeletal ultrasound and movement-based evaluation to help patients better understand their pain and return to the activities that matter most to them.





